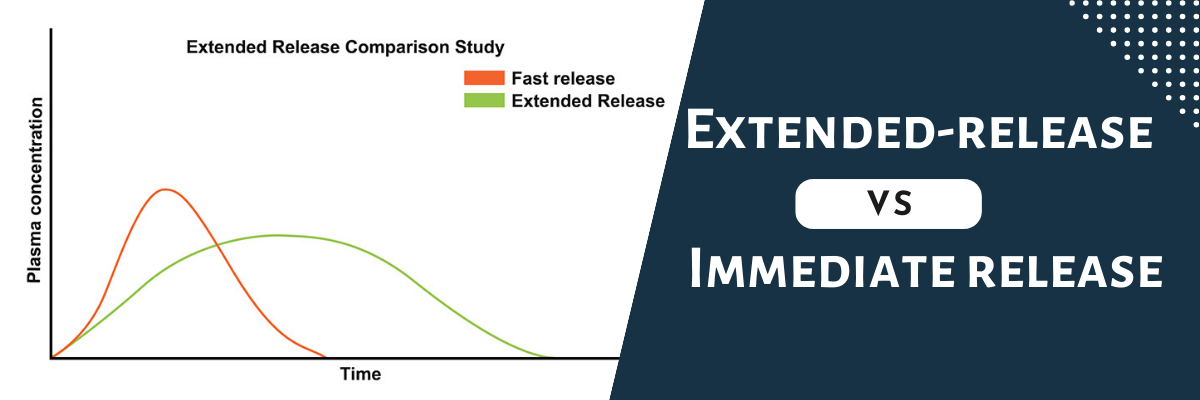
Ever stood in the pharmacy, prescription in hand, and wondered about the Extended-release vs Immediate release: making informed medication choices? Or perhaps you’ve sat across from your doctor as they explained your options. One pill lasts all day, another needs to be taken every few hours.
You’re not alone at this precipice of decision-making anymore, let’s embark on this journey together!
Table of Contents
Understanding Extended-Release and Immediate-Release Medications
Definition of Extended-Release Medications
Benefits and Drawbacks Of Immediate-Release Medications
Moving on to immediate-release (IR) counterparts – these are more like a shot of espresso. The full dose is released immediately after ingestion, quick fix you might say? Well yes, but this also means more frequent dosing which may not always be convenient or desirable due to potential side effects.
Evidence Base For Immediate Release-Medications
Drawing the Line: Extended-Release vs Immediate-Release
Let’s explore these nuances further.
Exploring the Effectiveness of Extended-Release and Immediate-Release Medications
Efficacy of Extended-Release Medications
The beauty of extended-release medications is that they offer a steady release of their active ingredients over time. This consistency can be particularly beneficial for managing chronic conditions such as diabetes or hypertension. Think about it as having a trusted friend who always remembers to water your plants while you’re away – consistent and reliable.
APA clinical treatment guidelines also suggest that certain mental health conditions may respond better to extended-release formulations due to their steady delivery method.
According to the CDC, antidepressants are the second most commonly prescribed drug in the United States, many of which come in an extended-release format.
Safety Profile Of Immediate-Release Medications
The Impact on Patient Outcomes: A Balancing Act
So, the next time your doc hands you a prescription, make sure to ask “Is this an extended-release or immediate-release medication?” and also inquire about how it works.
Considerations for Specific Clinical Conditions
Bone Health Medication Choices
Extended-Release for Mental Health Conditions
Immediate Release for Cardiovascular Disease
Factors Influencing Medication Choices
Role of Evidence-Based Guidelines
This gap suggests that there’s more work to be done in communicating about such tools. Patients should know their choices aren’t random, they’re based on solid evidence.
The Power of Patient Autonomy
Health Insurance: The Silent Decision-Maker
Last but certainly not least, we need to talk about cost sharing via health insurance plans. Many times it isn’t the effectiveness or side effects that drive our drug selection, instead it’s how much our wallet has to cough up.
Addressing Patient Concerns and Side Effects
Medication Adherence
Patient Experiences With Weight Gain on Extended-Release Medications
Mental Health Side Effects Of Immediate-Release Medications
Making Informed Medication Choices
Patient Experiences
Evaluating Research Studies for Medication Choices
An essential step in making informed choices about medication involves evaluating research studies. Such analysis requires looking beyond catchy headlines or attention-grabbing stats; instead, you need to dig into methodology, sample size, conflicts of interest, and other critical aspects of study design which could influence results.
FYI: It’s not always easy. For instance: “Antidepressants are the second most commonly prescribed drug in the United States”. This statement from CDC doesn’t provide insights into why these drugs are so prevalent nor does it give any hint towards their efficacy versus safety profile.
Understanding Guideline-Development Process
Accessing Health Care and Treatment Alternatives
Overcoming Barriers: Accessing Extended-Release Medications
A Look Beyond Medication: Non-Medication Treatment Options
Treatment doesn’t stop at medication, non-medication alternatives can also play a significant role in managing various clinical conditions effectively.
- CBT has been demonstrated to be an efficacious means of treating mental disorders without the need for medication.
- Physical exercise and a balanced diet can help manage conditions like diabetes or high blood pressure.
- Meditating and being mindful can be beneficial for mental well-being.
Navigating the maze of “Extended-release vs Immediate release: making informed medication choices” can be complex, but you’re now armed with knowledge. Remember that your unique health needs and preferences play a critical role in this decision.
Remember also to consider how long-term use may impact overall health. It’s not just about immediate relief, but ensuring sustained wellbeing too.
Evidence-based guidelines are there to help guide us. They provide insights on efficacy and safety profiles of these medications for different clinical conditions.
Above all, remember patient autonomy is key in selecting between extended-release and immediate-release medications. You have a voice, let it be heard!
FAQs in Relation to Extented -Release vs Immediate Release: Making Informed Medication Choices
What are the 3 principles of shared decision making?
Shared decision-making is based on three main pillars: information sharing, deliberation and implementing the agreed-upon choice.
What are the three types of medication review?
The three common types of medication reviews include prescription review, compliance assessment and clinical medication review.